Epidurals & Labor: Risks, Rewards, and More
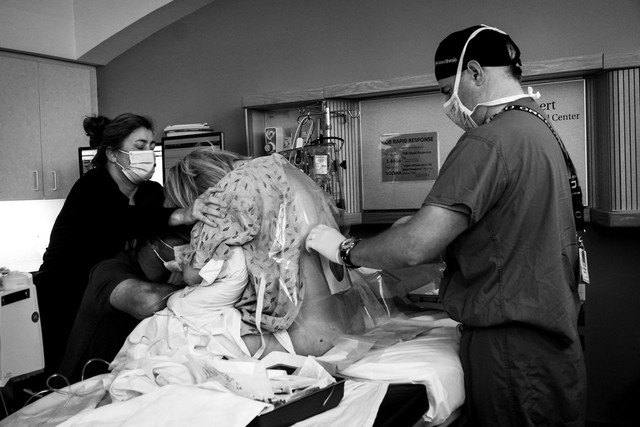
Have you considered how you’ll walk through surges and discomfort on your labor journey? In this post, we’re talking about all things EPIDURAL, the most common pain management tool offered during labor.

Cherry Blossom Doulas philosophy is a balanced approach to holistic/medical interventions. Our recommend is always to start off with the least amount of interventions, and work our way mindfully through medical options when desired and/or needed.
Let’s start with two scenarios
You come to us and are dead set on getting an epidural. Labor progresses too quickly, sometimes you request and receive it – and, it doesn’t work or you find yourself in a sea of unwanted interventions because of it. This can lead to disappointment and potential birth trauma.
In the same breath, another client comes to us and is dead set on having a completely unmedicated birth, but then is laboring for multiple days and has reached full exhaustion; this client has a mal positioned baby and is experiencing terrible back labor; they aren’t making cervical dilation progress; or they’ve changed their mind for any reason. This too can lead to disappointment and potential birth trauma.
This is why we ALWAYS recommend:
- have goals
- get educated on all of your options, and
- stay flexible with any changes that may be necessary, in any direction that might come

The BRAIN Acronym for Decision Making
Let’s break this conversation up using our favorite acronym.
B – What are the BENEFITS?
R – What are the RISKS?
A – What are ALTERNATIVES?
I – What does your INTUITION (listen and lean in)? and
N – What happens if we do NOTHING?
Benefits
An epidural can provide much needed rest, pain relief from contractions, reduce anxiety, allow the pelvic floor to relax (which can help with the progression of labor/cervical dilation), lower blood pressure (which is helpful with eclamptic/pregnancy induced hypertension), and can be helpful for those with sexual trauma in their past to help lessen the sensations of cervical exams/birthing.
Risks
An epidural does not always provide full coverage and pain relief. It can slow or stall your labor, which may result in needing other interventions (Pitocin, Vacuum, or Cesarean). It can cause anxiety because you are no longer able to move the lower half of your body. It decreases position options since you’re stuck in bed. It can decrease your blood pressure too much (which is counteracted by iv fluids). And, it can increase the chance of tearing during pushing, since you don’t know how much pressure to use. Additionally, it can cause a spinal headache.
Not everyone that wants an epidural is a good candidate. The most common contraindications include: you’ve progressed too far to receive the epidural; spinal abnormalities; coagulopathy/trouble clotting; infection at the injection site; neurological disease, etc. (Note: Beyond speaking with your doula about your goals, an informed provider can help navigate these hurdles ahead of time.)

Alternatives
- childbirth education (out-of-hospital preferred; as hospitals focus on hospital policy, not your goal)
- comfort measures
- position changes
- nitrous oxide
- protecting your sleep/resting in early labor
- nutrition and hydration to help your body labor efficiently
- iv pain medications
- doula support
- guided meditations
- hypnobirthing classes/tracks, and
- encouragement from your support people (which may include your partner, doula, and provider)
Intuition
This can be tricky when you are in the throes of active labor. Fear will automatically increase how you perceive pain. (Emotional and physical.) As your doula, we discuss how to navigate these tender, emotionally charged spaces.
Special Doula Tips
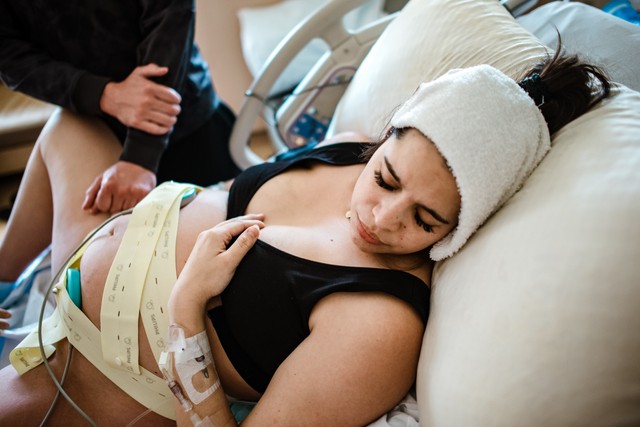
- Create a safe word that only you and your partner know that does not include, “I want an epidural.” Sometimes we say this but don’t actually want it, so having an unrelated word can help us know if and when you have reached your limit
- Stay flexible
- Labor as long as you can without medications by moving into multiple upright positions
- Wait until active labor (5-7 cm) to decrease the chances of needing other interventions from the epidural slowing labor down
- Stay open to position changes/comfort measures
- Know what your options are ahead of time
- Communicate to your partner and birth team about how you would like to navigate your goals for pain management – including what you would like to use and in what order
- Request not to have pain medication offered unless you ask for it
Nothing
The number two questions we ask as your doula are 1.) are you MANAGING (overall) and 2.) are you PROGRESSING (overall)? If the answer is yes to both, then we recommend to keep doing what you are doing: changing positions, changing comfort measures, encouraging, ensuring you are nourished and hydrated.
You can always change your mind and be 100% supported in your decision making process.
We are here to support YOUR JOURNEY in the most mindful and loving way. Whether that’s a planned cesarean, planned epidural, or planned unmedicated birth, we want to provide as much education, as many options, and un-biased support as humanly possible so that you leave your birth experience feeling respected and heard.
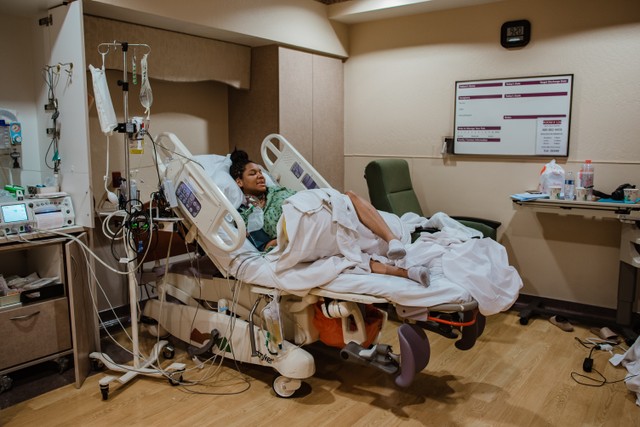
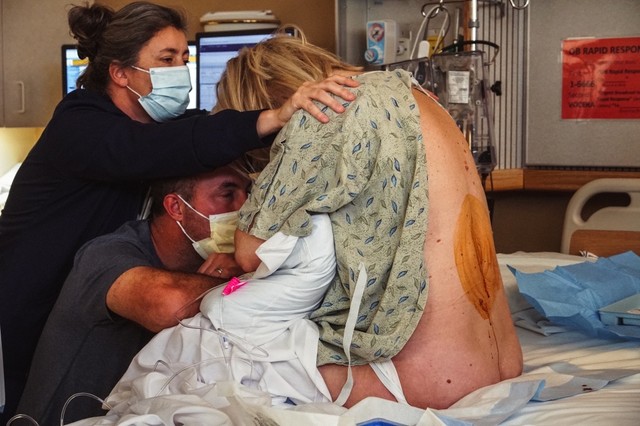
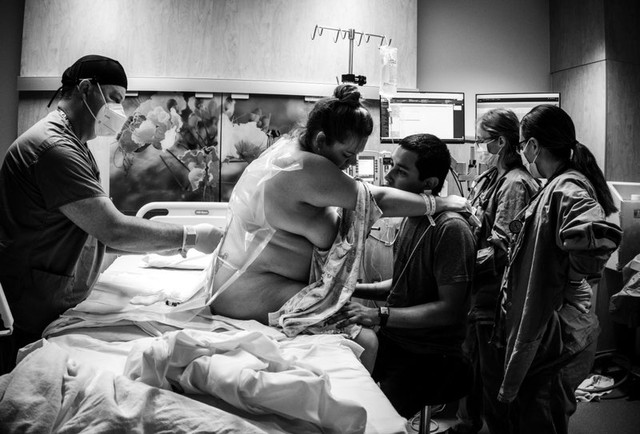
Epidural photography captured by our Cherry Blossom Doulas. To learn more about Epidurals, please go to our favorite evidenced based resource. For questions about doula support, please click here.

Hi! I’m Alyssa Leon. I lead Cherry Blossom Doula Services, LLC – an inclusive birth + postpartum doula team in Arizona; and mentor doulas in Arizona and beyond.